Sport Rehabilitation and Physiotherapy for De Quervains Tenosynovitis
What is De Quervain’s Tenosynovitis?
Inflammation of two tendons and the surrounding sheath at the base of the thumb making it difficult for the tendons to move smoothly. It is more common in women aged between 30 – 50 and may occur in both wrists. It may also be associated with diabetes, pregnancy and thyroid disease.
What Causes De Quervain’s Tenosynovitis?
It may occur due to direct trauma but the main cause is thought to be due to repetitive activities that involve repetitive thumb movements.
What are the symptoms of De Quervain’s Tenosynovitis?
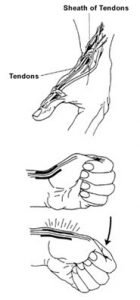
Pain at the base of the thumb particularly when gripping, wringing, pinching or lifting and sometimes there is a soft pocket of swelling. There may be grating (crepitus) during wrist movements and a test called Finkelstein’s test (as shown in the diagram) produces excruciating pain. If left untreated scar tissue can cause fibrosis of the soft tissues.
What will treatment consist of for De Quervain’s Tenosynovitis?
Massage – Encompassing a variety of techniques with sufficient pressure through the superficial tissue to reach the deep lying structures. It is used to increase blood flow, decrease swelling, reduce muscle spasm and promote normal tissue repair.
Deep friction – An aggressive massage technique applied across the tissue as deeply as possible to break down scar tissue, restore normal movement and prepare the structure for mobilisation or manipulation. This technique is initially painful but then causes a numbing effect.
Mobilisation – A manual technique where the joint and soft tissues are gently moved by the therapist to restore normal range, lubricate tissues and relieve pain.
Ultrasonic Therapy – Transmits sound waves through the tissues stimulating the body’s chemical reactions and therefore healing process, just as shaking a test tube in the laboratory speeds up a chemical reaction. It reduces tissue spasm, accelerates healing and results in pain relief.
Interferential Therapy – Introduces a small electrical current into the tissues and can be used at varying frequencies for differing treatment effects. E.g. pain relief, muscle or nerve stimulation, promoting blood flow and reducing inflammation.
What other treatments could be used for De Quervain’s Tenosynovitis?
Acupuncture – An oriental technique of introducing needles into the skin to increase or decrease energy flow to promote pain relief and healing.
Bracing – Wearing a thumb splint during the acutely painful stage can protect the thumb from being aggravated.
Injection Therapy – Is a specialist procedure during which a non-harmful steroid and local anaesthetic are injected directly into the injured structure. It has a dramatic effect on removing inflammation and promoting healing. Your therapist might recommend an injection before “hands on” therapy is commenced.
Taping/Strapping – May be used if thought necessary to restrict abnormal movement and prevent further damage.
What can you do yourself to help De Quervain’s Tenosynovitis?
Active Rest – Keep active but avoid any aggravating factors particularly any dexterous activities involving the thumb.
Apply an ice pack – For a maximum of 20 minutes. A bag of frozen peas wrapped in a damp cloth works well because it moulds to the shape of the tissues. Ensure that you do not apply ice directly to the skin as this can cause an ice burn.
Contrast bathing – From 5 days’ post injury put the hand into a bucket of water as hot as you can withstand for 5 minutes followed by one with water as cold as you can withstand for 5 minutes’ repeat for approximately 20 – 30 minutes.
Exercise programme – This is the most important part of the rehabilitation. Your therapist will instruct you as to which exercises to begin with, when to add the others, as well as how to progress the exercises.
Medication – Ask your GP or Pharmacist for advice on the best medication for your condition.
What if treatment does not help or resolve De Quervain’s Tenosynovitis?
It is rare that physical therapy does not resolve this condition. In these cases a cortisone injection may be appropriate and in very extreme cases surgery. These options can be discussed with your therapist if appropriate.
If you think you may have this condition we would love the opportunity to show you our expertise in the treatment and management of this condition so – Please click here for details of how to contact us to book an appointment
If you are unsure whether you have this condition or you would just like to speak to somebody then please get in touch here or call 0161 745 7551 or 0151 515 2323.